Sleep Isn’t Equal: How Hormones Shape Differences Between Sleep in Women and Men

By Dr.Krista Austin, O2X Sleep Specialist
Sleep presents unique differences between women and men.
Objective measures show that women obtain better sleep than men, despite reporting poor subjective sleep. Across the lifespan, women experience more sleep disruption (nighttime awakenings) and are twice as likely to experience insomnia. However, women obtain a greater amount of sleep, including deep sleep.
In contrast, men spend more time in light sleep and are more prone to sleep disturbances related to breathing disorders. Poor-quality sleep in young men is driven by lifestyle factors, whereas poor sleep in young women is attributed to hormonal fluctuations across the menstrual cycle.
Women: Sleep changes across the month and lifespan
In premenopausal women, fluctuations in sex steroid hormones play a central role in sleep quality. Estrogen supports restorative non-rapid eye movement (NREM) sleep, while progesterone influences rapid eye movement (REM) sleep. During the follicular phase and around ovulation, women typically report better sleep quality and feeling more restored. In the luteal phase, rising progesterone increases sympathetic nervous system activity and, along with elevations in prolactin, contributes to sleep disruption. Frequent nighttime awakenings can also elevate cortisol, further disrupting circadian rhythms and compounding fatigue. Before menstruation, women also report poor sleep due to sex steroid withdrawal.
Hormonal contraceptive use can further influence sleep. Women using combination (estrogen and progesterone) oral contraceptives often show a reduced cortisol awakening response alongside elevated baseline cortisol and melatonin levels. These changes, combined with increases in core body temperature, can impair sleep quality. As a result, oral contraceptive users commonly report more insomnia, shorter sleep duration, and greater sleep disruption.
Across the lifespan, additional hormone-related factors further affect sleep. During pregnancy, hormonal changes and, particularly in the third trimester, increased risk of obstructive sleep apnea due to weight gain can disrupt sleep. Postpartum, prolactin remains elevated to support breastfeeding, and frequent nighttime awakenings can lead to ongoing sleep disruption, fatigue, and increased risk of postpartum depression. Later, during perimenopause and menopause, declines in estrogen and progesterone reduce both NREM and REM sleep. Hot flashes contribute to frequent awakenings and elevated cortisol, while chronically elevated prolactin may further increase heat storage and discomfort.
Differences in sleep-related hormones also exist between men and women. In real-world settings, women tend to have an earlier onset and greater amplitude of melatonin production than men. This earlier rise in melatonin, along with a faster decline in core body temperature, promotes earlier sleep onset. However, under controlled laboratory conditions where light exposure is standardized, these differences largely disappear, highlighting the influence of behavioral factors related to light exposure in daily life.
Men: It’s Less About Testosterone Than You Think
In men, the role of testosterone in sleep is not well understood. While poor sleep can impair the normal nocturnal rise in testosterone, testosterone itself does not appear to be a primary driver of sleep quality and duration. Instead, elevations in stress hormones such as cortisol and prolactin play a more consistent role in disrupting sleep.
In aging men with low testosterone who do not meet criteria for hypogonadism (total testosterone <300 ng/dL), high-dose testosterone replacement therapy has been shown to reduce both sleep quality and duration. Similarly, in men with sleep apnea, testosterone supplementation can worsen symptoms rather than improve sleep.
Overall, there is limited evidence that testosterone improves sleep in men without true hypogonadism. However, in men who clearly meet clinical criteria, low- to moderate-dose testosterone replacement can improve sleep. In clinical settings such as prostate cancer, androgen deprivation therapy often leads to insomnia, hot flashes, and night sweats. However, estrogen supplementation has been shown to alleviate night sweats, further highlighting the complex hormonal influences on men’s sleep.
Additional insight on the role of testosterone in men comes from conditions such as hyperprolactinemia, where elevated prolactin levels are associated with increased sleepiness and disrupted sleep architecture. Treatment with dopaminergic agonists improves sleep quality and reduces daytime fatigue, often with a secondary increase in testosterone if it had been previously suppressed.
The following case highlights the interactions among sleep, hormones, and nutrition. A Special Forces operator presented with poor sleep quality, reduced sleep duration, high fatigue, and decreased physical performance. Evaluation revealed sleep apnea and elevated prolactin levels (identified through a thyrotropin (TRH) stimulation test). These abnormalities were attributed to traumatic brain injury from taking repeated IEDs.
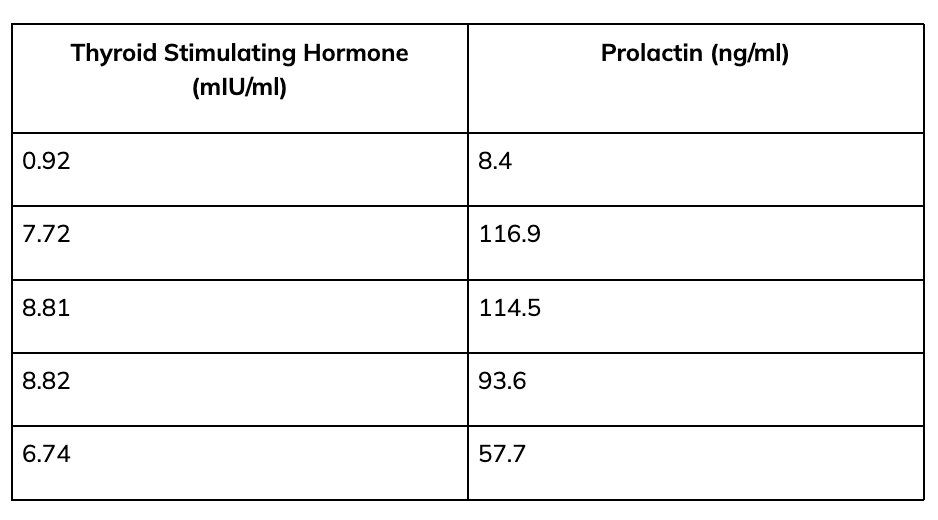
Treatment included continuous positive airway pressure (CPAP) for sleep apnea and a dopaminergic agonist to reduce prolactin. As sleep quality improved, fatigue resolved and physical performance returned.
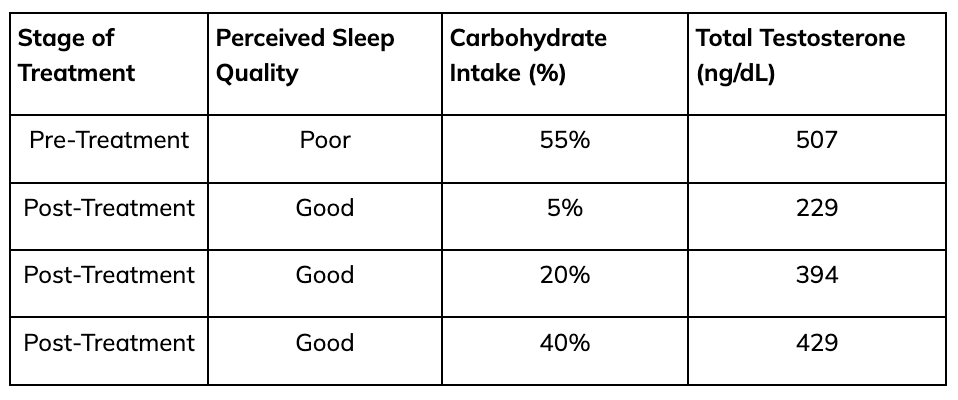
The Special Forces Operator chose to then assess testosterone again to see if it had risen. However, testosterone had fallen dramatically despite sleeping well and feeling physically better. Further assessment showed the operator had initiated a ketogenic (low-carbohydrate) diet, which is what lowered his testosterone levels. As carbohydrate intake increased, testosterone levels rose proportionally, independent of sleep quality.
Takeaway: Sleep restoration did not drive testosterone recovery; nutritional intake, specifically carbohydrate availability, is the primary factor for supporting testosterone.
Summary
In women, sleep is shaped by dynamic hormonal changes across the menstrual cycle and lifespan. In men, sleep disruption is more often linked to breathing disorders and lifestyle factors than testosterone alone. Understanding these differences is essential for accurately identifying the root cause of sleep issues and improving performance, recovery, and long-term health in tactical populations.
References:
- Mong, J. A., & Cusmano, D. M. (2016). Sex differences in sleep: impact of biological sex and sex steroids. Philosophical transactions of the Royal Society of London. Series B, Biological sciences, 371(1688), 20150110. https://doi.org/10.1098/rstb.2015.0110
- Zeng, L. N., Zong, Q. Q., Yang, Y., Zhang, L., Xiang, Y. F., Ng, C. H., Chen, L. G., & Xiang, Y. T. (2020). Gender Difference in the Prevalence of Insomnia: A Meta-Analysis of Observational Studies. Frontiers in psychiatry, 11, 577429. https://doi.org/10.3389/fpsyt.2020.577429
- Whitney, M. A., Schultz, D. N., Huber, L. R. B., Finke, A., Fitzgerald, A., & Hyde, A. (2022). The effects of hormonal contraceptive use on sleep patterns in women of reproductive age. Annals of epidemiology, 74, 125–131. https://doi.org/10.1016/j.annepidem.2022.07.006
- Morssinkhof, M. W. L., Larsen, S. V., Ozenne, B., Nasser, A., Hvitved, S., van der Werf, Y. D., Penninx, B. W. J. H., Broekman, B. F. P., & Frokjaer, V. G. (2025). Cortisol dynamics and sleep quality: The role of sex and oral contraceptive use. Psychoneuroendocrinology, 178, 107497. https://doi.org/10.1016/j.psyneuen.2025.107497
- Cignarelli, A., Castellana, M., Castellana, G., Perrini, S., Brescia, F., Natalicchio, A., Garruti, G., Laviola, L., Resta, O., & Giorgino, F. (2019). Effects of CPAP on Testosterone Levels in Patients With Obstructive Sleep Apnea: A Meta-Analysis Study. Frontiers in endocrinology, 10, 551. https://doi.org/10.3389/fendo.2019.00551
- Miao, X., Fu, Z., Luo, X., Wang, J., Yuan, L., Zhao, S., Feng, Y., Huang, S., & Xiao, S. (2024). A study on the correlations of PRL levels with anxiety, depression, sleep, and self-efficacy in patients with prolactinoma. Frontiers in endocrinology, 15, 1369729. https://doi.org/10.3389/fendo.2024.1369729
- Binar, M., Karakoc, O., Haymana, C., & Arslan, H. (2019). Cabergoline treatment in prolactinoma: Amelioration in obstructive and central sleep apneas. Journal of postgraduate medicine, 65(1), 47–49. https://doi.org/10.4103/jpgm.JPGM_113_18
About O2X Sleep Specialist Dr. Krista Austin:
Dr. Krista Austin is a Human Performance Specialist with more than 25 years of experience advancing resilience, recovery, and readiness across elite sport, tactical, and high-performance environments. She combines scientific rigor with practical application to help individuals and organizations perform at their best under pressure. Krista earned her Ph.D. in Movement Science from Florida State University and is a Certified Strength and Conditioning Specialist (CSCS) through the National Strength and Conditioning Association. Her diverse career spans leadership and consulting roles with the U.S. Olympic & Paralympic Committee, English Institute of Sport, and multiple U.S. national governing bodies, where she served as High Performance Director. She has also consulted for professional sports organizations, helping teams integrate evidence-based performance, nutrition, and recovery strategies to optimize athlete health and success. In the tactical domain, Krista has supported military research organizations and elite military units, developing performance solutions to enhance readiness and resilience in high-stress environments. Her work bridges research and operational practice, focusing on the human factors that drive sustained performance and recovery. At O2X, Krista specializes in the science of winning with a focus on sleep to optimize resilience helping tactical professionals understand how sleep impacts physical readiness, decision-making, and long-term health. She provides education that empowers individuals to improve sleep quality, enhance resilience, and maintain mission effectiveness in demanding environments.










